

















Motivation delivered to your inbox
Conditions Treated
Mold is a real threat, and we take it seriously. We offer comprehensive mold testing and treatment.
Struggle no more. Let us help you kick-start your body’s metabolism for effective weight loss.
Combatting fatigue, shortness of breath, brain fog, joint pain, and headaches with personalized care.
Experiencing flu-like symptoms, sleep disturbances, pain, or gastrointestinal issues?
Healthcare Services
Hormone imbalances? Our Hormone Replacement Therapy is designed to safely get you back on track.
Our IV Therapy harnesses the speed of intravenous delivery to infuse your body with elements.
Experiencing flu-like symptoms, sleep disturbances, pain, or gastrointestinal issues?
Your appointments go beyond generic advice. Benefit from a tailored plan of care.
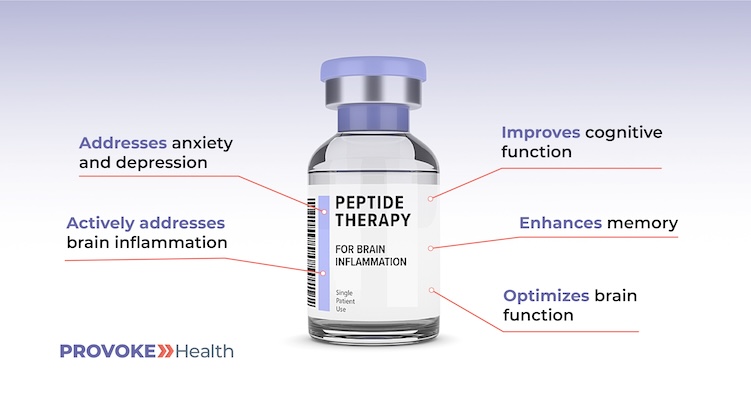
The Power of Peptides in Reducing Brain Inflammation
Weight Loss Benefits — and Side Effects — of Semaglutide and Ozempic
provoke (verb)
/pra vok/
1. An activator of change, sparking the of flames of proactive health action.
2. A catalyst that challenges traditional health norms and inspires unconventional thinking.
Provoke isn’t just a word; it’s a rallying cry for change. Who knew single idea could provoke such a shift in health consciousness? It’s the bold push towards embracing change and daring to think beyond the usual bounds.











